What Is The Survival Rate For Post Op Thoracic Aortic Repair Due To Aortic Rupture
Abstract
The aims of the study are to depict the long-term survival of patients undergoing chief open up ascending aortic surgery and to portray the development of aortic surgery during vi decades in a single centre. Included were all 614 patients who underwent principal ascending aortic surgery in 1968–2014 at i Nordic university hospital. Patients were identified and data were collected from patient records and surgical logs. Mortality information were acquired from the national registry. Median follow-up was xi.2 years using reverse Kaplan–Meier method. Overall 30-day survival was 91.2% and for xxx-24-hour interval survivor rates were 86.ix, 77.6, 52.1, 38.3 and 26.seven% at v, 10, 20, 30 and 40 years. There was no significant difference in long-term survival for 30-day survivors (p = 0.105) between patients treated emergently for dissection/rupture and electively (mainly ascending aortic aneurysms). On Cox regression era of surgery (p = 0.006), increasing age (p < 0.001) and indication (p < 0.001) were predictors of 30-solar day mortality. Arch involvement indicated twofold risk (Hour two.09, p = 0.05) compared to non-arch involved. Only increasing age (p < 0.001) predicted long-term mortality. There was a sixfold risk of 30-day bloodshed in the primeval era compared to the latest (p = 0.03). After the early postoperative phase post-obit ascending aortic surgery, the surgical indication and urgency of the index performance have no pregnant impact on long-term survival. The very long term survival after ascending aortic surgery is excellent for xxx-mean solar day survivors and improved through the era. Surgical treatment has improved and perioperative mortality has decreased significantly in 47 years.
Introduction
Thoracic aortic diseases (TADs) have increased steadily in recent years. The almost common diseases are aneurysms, dissections or ruptures. The annual incidence of thoracic aortic aneurysms and dissections has previously been estimated at 16.3/100,000 for males and 9.1/100,000 for females, with an increasing trend in recent years [1]. Previous studies have established historic period, atherosclerosis, hypertension, the bicuspid aortic valve, connective tissue diseases such as Marfan syndrome or Ehlers–Danlos syndrome, previous cardiac surgery and family history as risk factors for thoracic aortic aneurysms (TAAs) and ascending aortic dissections (AADs) or ruptures. It is known that the size of the aorta correlates with the gamble of complications [2] and the current guideline-based threshold for surgical intervention is aortic bore ≥ 5.5 cm, regardless of aetiology [4]. Once dissected, the mortality for those surviving until surgical theatre has been reported at 25.1% [3]. If ruptured, the overall mortality reaches over 94% [5].
Cooley and DeBakey performed the first successful ascending aortic resection in 1951 using an allograft and on cardiopulmonary bypass [6]. The surgical techniques take since adult over the years. Many studies have shown that both postoperative in-hospital and later mortality for ascending aortic dissections (blazon A) accept significantly decreased in contempo years [seven,8,ix,10,eleven,12]. Withal, the follow-up periods have mostly been short and very few clinical studies accept been conducted to evaluate the long-term outcome of TADs for those who survived the disquisitional initial 30-twenty-four hours period.
Due to the relatively low prevalence of TADs, and the relatively late adoption and evolution of operative handling, long-term survival subsequently TAD surgery still remains unclear. The purpose of this study is to investigate short- and long-term mortality after surgical handling of ascending thoracic aortic diseases and to depict the evolution of ascending aortic surgery over the form of six decades.
Materials and methods
This is a retrospective study consisting of all 614 consecutive patients who underwent primary ascending aortic surgery in a single centre, Turku University Infirmary, Southwest Finland, betwixt 1968 and 2022. Patients who underwent ascending aortic and/or aortic arch surgery with or without descending aortic surgery were included.
For estimation of postoperative mortality, patients who deceased during functioning were excluded, following recommendations for reporting results after valvular surgery by the guidelines of the American Association for Thoracic Surgery, The Society of Thoracic Surgeons, and the European Association for Cardio-Thoracic Surgery [13].
The current geographical catchment area of TAD operations in Turku university hospital was established in 1984; therefore, we included only patients from 1984 to 2022 for population incidence calculations. The incidence concerns but surgically treated TAD patients aged ≥ 18 years. Incidence was standardized using the 2000 U.s.a. Standard population with direct method.
Baseline data were collected retrospectively from patient records and surgical logs. One patient (1/614) was lost during the follow-upwardly. The mortality and population data were provided past the Finnish national registry, Statistics Finland.
Due to the long follow-up, timing of surgery was classified into iv eras: 1968–1980 (as there were only half-dozen patients during 1968–1970), 1981–1990, 1991–2000 and 2001–2014. Age was classified into ≤ 40 (14.7% of patients), 41–50 (xiii.ix%), 51–60 (27.five%), 61–70 (29.iv%) and ≥ seventy (14.four%) years. Four categories were created according to the surgical arroyo that was used or intended to use on the patient: modified Bentall process which involves replacement of the ascending aorta and aortic root with a composite tube graft and valve prosthesis (biological or mechanical) and coronary reimplantation as described by Inberg et al. [14]; modified Bentall process with concomitant coronary bypass (CABG) and/or mitral valve replacement (MVR) was classified as modified Bentall + CABG/MVR; valve-sparing David or Yacoub procedure with coronary reimplantation; isolated interposition with a tube graft of the ascending aorta and lastly hemiarch if the inner curvature of the aortic arch was replaced or total arch if distal anastomosis lied distal to the left subclavian artery with arch vessel reimplantation either separately or as islands. The indication for surgery was classified into those who had acute or chronic ascending aortic dissection, aortic rupture or intramural haematoma (i.eastward. aortic emergencies), and those who had other elective indications (namely TAA with or without aortic insufficiency). Survival analysis included only patients alive after performance and reoperations consisted of either resternotomies within the same hospital period or reoperations requiring a resternotomy after hospital discharge.
The written report was canonical by the institutional review board.
Statistics
Chi-squared tests were conducted to depict interactions betwixt historic period, sex, era of surgery, operation numbers, indication for operations and surgical approaches. Kaplan–Meier survival estimates were used for the long-term survival for 30-solar day survivors. The survival was also explored past indication and by decade of the surgery. Log-rank examination was used to test the differences betwixt the groups. Cox proportional hazards regression modelling was conducted to identify predictors of the brusk- and long-term mortalities. p values < 0.05 were inferred statistically significant. All statistical analyses were performed with SPSS IBM Statistics version 22.0 (IBM, Armonk, NY, United states of america).
The evolution of surgical techniques
In the 1970s, a modified Bentall technique, as described by Inberg et al. [14], was adopted in Turku academy hospital for reconstruction of the root and ascending aorta and thereafter was used equally the preferred approach for root replacement in both astute and elective cases. In cases of a competent valve and minimal root involvement, an isolated supracoronary replacement of the ascending aorta was used. Hemiarch and total curvation replacements were adopted in the 2000s for pathologies of the ascending aorta and were rarely used in earlier years. Valve-sparing (David) techniques for root surgery were adopted in 2009 and used thereafter for suitable constituent cases.
Until the tardily 1990s, cannulation was performed with direct cannulation of a femoral artery for acute aortic dissection. Thereafter, the almost common arterial cannulation was switched to cannulation through an 8-mm cease to side vascular prosthesis to the femoral artery. In save cases, however, straight cannulation was still employed for rapid access. For elective cases, arterial cannulation was located at the lesser curvature of the curvation for ascending aortic surgery and femoral artery for arch repair. Venous drainage was achieved either through the femoral vein or right atrium. Directly selective cannulation of supra-aortic vessels was used for arch repair.
Hypothermia for elective cases of ascending aortic surgery was at 30–34 centigrade and until the mid-2000s, the ascending aortic surgery was performed on-clamp. Total circulatory abort and deep hypothermia (xx–24 degrees centigrade) with open distal anastomosis was adopted forth with hemiarch repair during 2000s. Deep hypothermia and circulatory arrest with selective antegrade cerebral perfusion was used for arch repair during acute setting.
Results
The total study population consisted of 614 patients who had undergone an ascending aortic operation. The median follow-up was 11.8 years using reverse Kaplan–Meier method (range 0–46.viii) for the entire accomplice, and the overall mean age at the time of surgery was 56.0 ± 14.iv years (range xviii–84). As shown by Tabular array one, the average historic period increased significantly (p < 0.001) for patients undergoing ascending aortic operations over the decades: less than 40 years onetime decreased from 48.0 to 10.0%, from the 1960s to the 2022s, respectively, while at the same time the proportion of over 70 years old increased from 0.0 to 25.4%. Of all patients, 33.seven% were treated for aortic dissections or ruptures, the rest 66.3% had mainly elective aneurysms. The number of males who underwent TAD surgery was fourfold compared to females (n = 491, 80% vs. n = 123, xx%), but females tended to have more dissections and ruptures than males (p = 0.023).
The number of surgically treated TADs increased steadily from an average of iii.8 operations per yr in the 1960s and 1970s to 32.5 operations per yr in the 2022s (Fig. 1). During 1984–2014, the incidence of surgically treated TADs was 0.96 cases per 100,000 per year for females, 4.72 cases per 100,000 per year for males and overall 2.78 per 100,000 inhabitants per twelvemonth. The incidence increased significantly from 1984 to 2022 in both sexes, from i.68/100,000/year in 1984–1990 to 4.80/100,000/year in 2022–2014. The increase was more prominent for females than for males (0.45–i.95 per 100,000 vs. ii.98–7.76 per 100,000) (Fig. 2). The Bentall procedure has remained the most frequent surgical arroyo, at an average of 59.8% of all surgeries. In the 1968–1980 supracoronary replacement of the ascending aorta with a tube graft (i.e. interposition) was the most employed approach of all (49.0%) simply dropped notably towards the twenty-first century (xiv.6%).
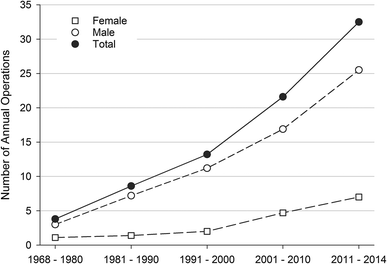
Annual number of operated ascending aortic diseases per decade
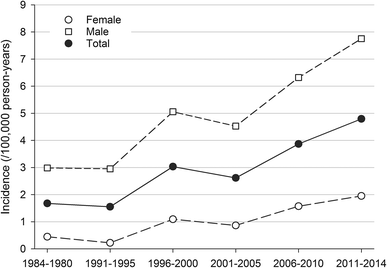
Average sex-specific incidence rate per decade per hundred thousand inhabitants for operated ascending aortic diseases (1984–2014)
Postoperative survival
Among all those who survived the index procedure, the postoperative survival was 86.8, 79.5, 70.3, 47.one, 34.half-dozen and 24.two% at 1, 5, 10, xx, 30 and 40 years after operation, respectively. In full, 223 patients (39.half-dozen%) died during follow-upwardly from 1968 to 2022. Postoperative 30-mean solar day bloodshed was 9.2% overall, 18.three% (OR 1.75, CI ane.27–2.41) for emergent dissections or ruptures and 5.5% (OR 0.45, CI 0.35–0.60) for other indications (p < 0.001). For all patients who survived upwardly to hospital admission, the perioperative mortality was 7.5% and the thirty-twenty-four hour period mortality charge per unit was xvi.0%. The long-term survival for xxx-mean solar day survivors was 86.nine, 77.half-dozen, 52.1, 38.three and 26.7% at five, x, 20, xxx and 40 years. The hateful survival afterward thirty days was 10.four years (median 7.7, SD ± 9.v, interquartile range 9.6–11.ii).
The Kaplan–Meier analysis with log-rank test showed a significant difference in 30-day bloodshed (p < 0.001) between patients treated emergently for dissection/rupture and electively for mainly aneurysms. There was no difference (p = 0.096) in long-term survival for those who survived the first xxx days (Fig. iii). On a multivariable Cox proportional hazard model, increasing age and the indication for surgery predicted 30-24-hour interval mortality. At that place was a trend towards a greater bloodshed with arch involvement (p = 0.056). There was a sixfold hazard of thirty-day mortality in the earliest era of TAD surgery compared to the latest era (1968–1980 vs. 2022–2014, 60 minutes six.0, p = 0.002). For long-term survival for 30-24-hour interval survivors, increasing age was the only significant predictor for mortality (p < 0.001) (Table 2).
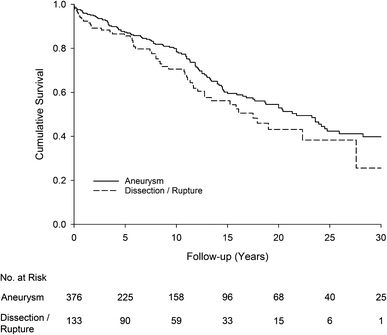
Kaplan–Meier survival curve for 30-day survivors stratified by surgical indication: acute dissection/rupture vs. elective surgery (mainly aneurysms). There were no statistical difference in long-term survival between the groups (p = 0.096). Numbers at risk are indicated
Reoperations
The cumulative incidence of postoperative resternotomy during the same hospital menses was 3.2% (n = 18). Cumulated incidence of reoperation after hospital belch was 2.3% (n = 13), of which four patients (25%) died during reoperation. Freedom from reoperation was 98.1, 98.1, 95.6, 94.0 and 86.2% at 5, 10, 20, 30 and forty years. The indication for reoperations was thoracic aortic aneurysm (northward = 3), abdominal aortic aneurysm (north = 2), aortic dissection (due north = two), chronic pericarditis (north = two), arrhythmia (due north = 2), thoracic aortic rupture (n = 1), abdominal aortic rupture (northward = 1), mechanical valve infection (n = i), aortic valve stenosis (n = 1), mitral valve regurgitation (n = one), coronary avenue disease (north = i) and coronary artery aneurysm (n = 1).
Word
To our cognition, this is the longest follow-up of patients treated surgically for ascending aortic diseases, starting from the very get-go ascending aortic operation performed in Republic of finland in 1968 continuously until 2022, 47 years in full with 100% completeness of follow-up. We describe 6 decades of aortic surgery and draw trends in surgical approaches in both brusque-term and very long-term survival.
In previous studies, the late survival for infirmary survivors has been reported lower for acute dissections [9, ten, 15, 16]. In a Swedish nationwide population-based study the survival for > 30 days from operation for both aneurysms and dissections was 77, 57 and 43% at 5, 10, and 15 years, respectively [1]. Our total follow-upward was more than 30 years longer and the survival rate was higher. In improver, the perioperative and initial thirty-day mortality of aortic dissections are also comparable with a previous study [17].
Interestingly, our data showed no difference in long-term survival for 30-day survivors, regardless of aetiology. Our results suggest that surgical indication and approach have piffling effect on long-term prognosis; if patients survive the disquisitional 30-24-hour interval postoperative period, long-term survival for ascending aortic dissections or ruptures appears to be every bit skillful equally for ascending aortic aneurysms.
Postoperative resternotomies during the same infirmary admission were surprisingly exceptional and the rate of reoperations later on belch was fifty-fifty lower in our data, also indicating fantabulous surgical result. Previous studies have reported reoperation charge per unit to be from 7.viii to 23.2% and that reoperation rates were non associated with preoperative aortic regurgitation severity, surgical technique nor any other factors for that matter [one, 10, 18]. Reoperations are technically challenging due to tight adhesions and the mortality however remains high specially for distal re-dos [nineteen]. It tin exist speculated that bodily indications for reintervention on the aorta are hitherto unclear and represent subjective institutional and surgeon-dependent thresholds for surgery, but farther studies on discipline are warranted. Nonetheless, our late reoperation rates should be interpreted with caution equally possible reinterventions performed at other institutions cannot be completely deemed for even if treatment of ascending aortic pathologies is centralized inside geographic areas in Finland. Nevertheless, information technology is unlikely that the number of reoperations unaccounted for in these data would exist dramatic.
We found a steady increase in incidence of TAD operations over past six decades for both sexes. Similar trends accept been described by several previous studies likewise [1, seven, 20]. This study, similar almost previous studies, describes only the incidence of operated TADs and did non include patients who were treated conservatively or who died prior to infirmary admission. Thus, the true incidence of TADs is expected to be higher than reported hither, or previously, due to its predominantly silent grapheme and high pre-hospital mortality during an astute issue. In fact, according to a previous study, 95% of TADs were reported asymptomatic before an acute event, such as dissection or rupture [21]. Improved imaging techniques and their improve availability in addition to meliorate awareness and understanding of the disease have improved the diagnostics of TADs, only whether the true incidence of TAD has increased lately remains unclear.
Very long outcomes of patients with ascending aortic diseases and especially ascending aortic aneurysms have not been extensively described. Previous studies accept mostly been either longer follow-ups with few cases from a unmarried centre or short follow-ups with large information from centres specialized in aortic diseases. Our data consist of an extensively collected all-comers cohort from a tertiary centre that covers unselected patients in demand of aortic surgery in Southwest Finland. The current study describes real-earth outcomes, which are maybe ameliorate applicative to the majority of western cardiac surgical units than results from highly specialized aortic centres.
The immediate primary goal during an aortic catastrophe is to perform necessary operational care while ensuring survival. In smaller cardiothoracic centres, this is achieved past minimizing the complexity of the procedure. The more complex the procedure, such as elephant trunks in hybrid techniques afterward initial ascending aortic repair, the longer the patient has to exist nether perfusion and anaesthesia, leading to a higher charge per unit of postoperative ischemic events and early mortality. Information technology is also imperative that the techniques used are replicable past all cardiac surgeons performing on-call duties. Some studies have suggested that more than complex operations may atomic number 82 to better long-term survival and reduction in rates of reoperations [22,23,24]. Our study showed an extremely low charge per unit of reoperations and an splendid long-term survival after the initial 30 days.
Limitations
The major limitations of this unmarried-centre written report are associated with the retrospective nature of the database. Although data were checked straight from patient files, incompleteness is still a possibility. During decade-long follow-up, the evolution of surgical techniques, engineering, devices, and the improvement of perioperative and postoperative management have been radical, but this is too one the main focus of this study, i.eastward. the evolution of surgical management of ascending aortic pathologies.
Conclusions
Our study shows that a relatively modest cardiothoracic surgery centre can produce comparable results with specialized good centres in both emergent and constituent ascending aortic surgery. This puts into question the oft-suggested high-volume requirements for quality ascending aortic surgery. Our results besides advise that an initially straightforward and simple surgical approach yields skilful long-term prognosis indicating that a KISS (keep it brusque and simple) approach is justified in ascending aortic surgery.
References
-
Olsson C, Thelin S, Stahle E, Ekbom A, Granath F (2006) Thoracic aortic aneurysm and autopsy: increasing prevalence and improved outcomes reported in a nationwide population-based study of more than 14,000 cases from 1987 to 2002. Circulation 114:2611–2618
-
Chau KH, Elefteriades JA (2013) Natural history of thoracic aortic aneurysms: size matters, plus moving beyond size. Prog Cardiovasc Dis 56:74–80
-
Trimarchi Due south, Nienaber CA, Rampoldi V, Myrmel T, Suzuki T, Mehta RH, Bossone E, Cooper JV, Smith DE, Menicanti L, Frigiola A, Oh JK, Deeb MG, Isselbacher EM, Eagle KA (2005) Contemporary results of surgery in acute type A aortic dissection: the international registry of acute aortic dissection experience. J Thorac Cardiovasc Surg 129:112–122
-
2010 ACCF/AHA/AATS/ACR/ASA/SCA/SCAI/SIR/STS/SVM Guidelines for the Diagnosis and Management of Patients With Thoracic Aortic Disease Representative Members, Hiratzka LF, Creager MA, Isselbacher EM, Svensson LG, AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease Representative Members, Bonow RO, Guyton RA, Sundt TM 3rd (2016) Surgery for aortic dilatation in patients with bicuspid aortic valves: a statement of description from the american college of Cardiology/American heart association task force on clinical exercise guidelines. J Thorac Cardiovasc Surg 151:959–966
-
Johansson Thou, Markstrom U, Swedenborg J (1995) Ruptured thoracic aortic aneurysms: a written report of incidence and mortality rates. J Vasc Surg 21:985–988
-
Cooley DA, De Bakey ME (1956) Resection of unabridged ascending aorta in fusiform aneurysm using cardiac bypass. J Am Med Assoc 162:1158–1159
-
Pape LA, Awais Thousand, Woznicki EM, Suzuki T, Trimarchi S, Evangelista A, Myrmel T, Larsen M, Harris KM, Greason K, Eusanio MD, Bossone East, Montgomery DG, Eagle KA, Nienaber CA, Isselbacher EM, O'Gara P (2015) Presentation, diagnosis, and outcomes of acute aortic dissection: 17-year trends from the international registry of astute aortic dissection. J Am Coll Cardiol 66:350–358
-
Tsai TT, Evangelista A, Nienaber CA, Trimarchi South, Sechtem U, Fattori R, Myrmel T, Pape L, Cooper JV, Smith DE, Fang J, Isselbacher E, Eagle KA (2006) Long-term survival in patients presenting with type A astute aortic dissection: insights from the international registry of acute aortic dissection (IRAD). Apportionment 114:I350–I356
-
Higgins J, Lee MK, Co C, Janusz MT (2014) Long-term outcomes later on thoracic aortic surgery: a population-based study. J Thorac Cardiovasc Surg 148:47–52
-
Bekkers JA, Raap GB, Takkenberg JJ, Bogers AJ (2013) Astute blazon A aortic dissection: long-term results and reoperations. Eur J Cardiothorac Surg 43:389–396
-
Hysi I, Juthier F, Fabre O, Fouquet O, Rousse North, Banfi C, Pincon C, Prat A, Vincentelli A (2015) Aortic root surgery improves long-term survival later on acute type A aortic dissection. Int J Cardiol 184:285–290
-
Gaudino 1000, Lau C, Munjal G, Avgerinos D, Girardi LN (2015) Contemporary outcomes of surgery for aortic root aneurysms: a propensity-matched comparison of valve-sparing and composite valve graft replacement. J Thorac Cardiovasc Surg 150(1120–1129):e1
-
Akins CW, Miller DC, Turina MI, Kouchoukos NT, Blackstone EH, Grunkemeier GL, Takkenberg JJ, David TE, Butchart EG, Adams DH, Shahian DM, Hagl S, Mayer JE, Lytle BW (2008) Guidelines for reporting bloodshed and morbidity afterwards cardiac valve interventions. J Thorac Cardiovasc Surg 135:732–738
-
Inberg MV, Niinikoski J, Savunen T, Vänttinen East (1985) Total repair of annulo-aortic ectasia with composite graft and reimplantation of coronary ostia: a consecutive serial of 41 patients. World J Surg nine(3):493–499
-
Howard DP, Banerjee A, Fairhead JF, Perkins J, Argent LE, Rothwell PM (2013) Population-based written report of incidence and outcome of astute aortic dissection and premorbid risk factor control: x-twelvemonth results from the oxford vascular study. Circulation 127:2031–2037
-
Tan ME, Morshuis WJ, Dossche KM, Kelder JC, Waanders FG, Schepens MA (2005) Long-term results afterward 27 years of surgical treatment of acute blazon a aortic autopsy. Ann Thorac Surg 80:523–529
-
Colli A, Carrozzini Thousand, Galuppo Chiliad, Comisso Thou, Toto F, Gregori D, Gerosa Yard (2016) Assay of early and long-term outcomes of acute type A aortic dissection according to the new international aortic curvation surgery study group recommendations. Heart Vessels 31:1616–1624
-
Arabkhani B, Mookhoek A, Di Centa I, Lansac E, Bekkers JA, Van Wijngaarden RDL, Bogers AJ, Takkenberg JJ (2015) Reported outcome after valve-sparing aortic root replacement for aortic root aneurysm: a systematic review and meta-assay. Ann Thorac Surg 100:1126–1131
-
Dell'Aquila AM, Pollari F, Fattouch Thousand, Santarpino Thousand, Hillebrand J, Schneider S, Landwerht J, Nasso Thousand, Gregorini R, Giglio Medico, Mikus E, Albertini Am Deschka H, Fishlein T, Martens Due south, Gallo A, Consistre K, Speziale K, Regesta T (2017) Early on outcomes in re-do operation after acute blazon A aortic dissection: results from the multicenter REAAD database. Heart Vessels 32:566–573
-
Yeh TY, Chen CY, Huang JW, Chiu CC, Lai WT, Huang YB (2015) Epidemiology and medication utilization patterns of aortic dissection in taiwan: a population-based report. Medicine (Baltimore) 94(36):e1522
-
Kuzmik GA, Sang AX, Elefteriades JA (2012) Natural history of thoracic aortic aneurysms. J Vasc Surg 56:565–571
-
Roselli EE, Loor G, He J, Rafael AE, Rajeswaran J, Houghtaling PL, Svensson LG, Blackstone EH, Lytle BW (2015) Distal aortic interventions subsequently repair of ascending autopsy: the statement for a more ambitious approach. J Thorac Cardiovasc Surg 149(S117–124):e3
-
Pugliese P, Pessotto R, Santini F, Montalbano Grand, Luciani GB, Mazzucco A (1998) Take a chance of tardily reoperations in patients with acute type A aortic autopsy: Impact of a more radical surgical approach. Eur J Cardiothorac Surg 13:576–580 (give-and-take 580–i)
-
Murzi G, Tiwari KK, Farneti PA, Glauber M (2010) Might type A acute dissection repair with the add-on of a frozen elephant trunk improve long-term survival compared to standard repair? Collaborate Cardiovasc Thorac Surg eleven:98–102
Writer information
Affiliations
Respective authors
Ethics declarations
Conflict of interest
Emily Pan has no disclosures. Dr. Kytö has received scientific consultation fee from AstraZeneca. Dr. Savunen has no disclosures. Dr. Gunn has received unrestricted funding for educational congress expenses from St Jude Medical, Johnson & Johnson, AstraZeneca and Medtronic.
Funding
This study was supported by governmental VTR-funding of the hospital district of Southwestern Finland and grant funding of the Finnish Cardiac Society.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in whatever medium, provided y'all give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and bespeak if changes were made.
Reprints and Permissions
Virtually this article
Cite this article
Pan, Eastward., Kytö, V., Savunen, T. et al. Early and late outcomes later open ascending aortic surgery: 47-year feel in a single middle. Heart Vessels 33, 427–433 (2018). https://doi.org/x.1007/s00380-017-1075-iii
-
Received:
-
Accepted:
-
Published:
-
Upshot Date:
-
DOI : https://doi.org/10.1007/s00380-017-1075-3
Keywords
- Aorta
- Aortic arch
- Aortic dissection
- Aortic surgery
- Aortic root
- Outcomes
Source: https://link.springer.com/article/10.1007/s00380-017-1075-3
Posted by: houstonbeturped.blogspot.com


0 Response to "What Is The Survival Rate For Post Op Thoracic Aortic Repair Due To Aortic Rupture"
Post a Comment